Introduction
Have you thought about going back to school to become a nurse practitioner but have no idea where to start? Look no further. This article highlights key information, questions you may have about the role itself, educational pathways, and early career advice from one person’s journey to becoming a nurse practitioner and now a program director.
How long has the nurse practitioner role been around?
It is impossible to talk about the history of nursing without acknowledging Florence Nightingale and her role in the Crimean War. Prior to that, nursing care was attributed to a person’s family and friends. This progressed in the 19th century when education was structured like an apprenticeship with limited function and role, which was often seen as very demanding with very little reward. In the 20th century, the professional evolution continued with the baccalaureate degree, and evidence reflected better patient outcomes through this higher level of education and expanded roles beyond the bedside (ANA).
The first nurse practitioner program was developed in 1965 at the University of Colorado by Dr. Loretta Ford and Dr. Henry Silver. To further advocate for the role, the American Nurses Association (ANA) developed the Council of Primary Care Nurse Practitioners in 1974; and in the same year, through the Burlington Randomized Trial of the Nurse Practitioner, it was determined that nurse practitioners were safe and made appropriate referrals when medical intervention was necessary (Spitzer, 1974). Since that time, the nurse practitioner role and educational programs have continued to develop and grow — and, as of 2025, there are more than 461,000 nurse practitioners in the United States (AANP).
What exactly is a nurse practitioner?
A nurse practitioner is an advanced practice registered nurse (APRN) who is a clinician trained in the assessment, diagnosis, management, and treatment of patients with acute, chronic, and critical illness. They also have training in health promotion and disease prevention. They work collaboratively as part of the multidisciplinary healthcare team within the statutes of their state board of nursing defined scope of practice and their individual clinical practice site’s APRN practice agreements.
What is the Consensus Model?
The Consensus Model originated in 2008 to differentiate the four classifications of APRNs: nurse practitioner, clinical nurse specialist, nurse midwife, and nurse anesthetist. It aimed to standardize the regulation of APRNs across the United States.
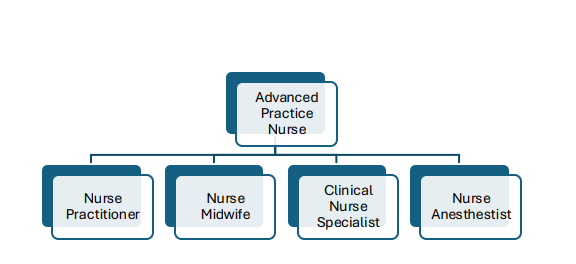
Image adapted from AACN Consensus Model Report: Report of the APRN Joint Dialogue Group Based on the Work of the APRN Consensus Group and the NCSBN APRN Committee
In addition, it provides guidance on licensure, accreditation, certification, and education to reduce inconsistencies between states.
What does the educational journey require to become a nurse practitioner?
As a nurse practitioner, your educational path requires you to choose a population focus and sometimes a practice setting for your specialty. This includes adult-gerontology acute care, adult-gerontology primary care, family, pediatric acute care, pediatric primary care, neonatal, or psychiatric-mental health. It is possible to complete a program in more than one specialty, especially if needed for the patient care environment in which you want to work.
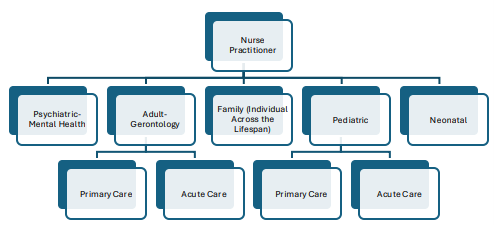
Image adapted from AACN Consensus Model Report: Report of the APRN Joint Dialogue Group Based on the Work of the APRN Consensus Group and the NCSBN APRN Committee
The minimum educational preparation to become a nurse practitioner is a Master of Science in Nursing (MSN), but you can also choose to pursue a Doctor of Nursing Practice (DNP). Both degree programs must contain the three Ps — pathophysiology, pharmacology, and physical exam — as well as a minimum number of clinical hours as set forth by the American Association of the Colleges for Nursing standards. Total program credits and course-specific work will vary by institution (AACN).
How do I know which educational program is right for me?
First, you must choose an accredited program that provides you with at least the minimum requirements to be eligible for board certification. Next, you should ensure the program is within your budget, especially if you will be unable to continue to work (or even at the level you have been) due to coursework and clinical time.
Regarding an on-site, hybrid, or fully online model — that is a question that only you as an adult learner can answer. You must ask yourself: How do I best learn, study, and retain information? If it is on-site or hybrid, do you have the means to travel during times of mandatory attendance?
How do I know which population focus or practice environment is right for me?
The first step is to shadow several nurse practitioners in any area you may have an interest in, even if it’s outside of your current bedside practice. You also should shadow nurse practitioners who work at your facility, and ones who don’t. This will give you greater insight into how unique and dynamic this role is and introduce you to practice and population settings you may want to pursue.
The clinical environment can vary between units and departments within the same facility, which is why shadowing can be so influential in your decision prior to starting school. This is also valuable again when you are ready to enter the job market to get a true idea of the role of the nurse practitioner within that department, from scheduling requirements to scope of practice and expectations of the role. There is no better insight than meeting and rounding with those who already work there to learn the strengths and opportunities for improvement that exist in that environment.
It is then during your clinical education where most providers solidify the practice environment they want to be (or at least the ones they don’t want to be) in as a nurse practitioner. There are certain requirements for your degree programs, so it is important to identify mandatory versus elective rotations during the program.
Who defines your scope of practice?
The scope of practice of a nurse practitioner is defined by the state in which you hold a license. Although the Consensus Model helps to reduce variations between states, variations still exist. This scope can also be further limited or modified based on the facility (acute care) or practice (primary care) in which you work.
Taking it one step further, there are variations to practice authority between states where nurse practitioners are defined as either having full practice, reduced practice, or restricted practice. This also exists with prescriptive authority, in which nurse practitioners are considered to have either restricted or unrestricted authority.
The two biggest impacts that these limitations have are: (1) they require the supervision and/or collaboration of a physician, and (2) they often limit a nurse practitioner in practice from the educational training they have completed.
The American Association of Nurse Practitioners offers a useful resource, Practice Information by State, where you can find information about the state where you reside.
Once I’m done with school, then what do I do?
This is where the L-A-C-E (Licensure, Accreditation, Certification, and Education standards) Model enters the picture. In short, accreditation is the formal review and approval of the minimum education standards (degree, coursework, clinical hours) required to sit for certification. Once certification is achieved, you can then apply for your individual state license, which will validate the education and certification that have been completed and grant you the authority to practice.
I’m certified and licensed as a nurse practitioner. How do I transition to practice?
Post-graduation, there are two paths that you can take. The first is to jump into the workforce, practicing as a nurse practitioner. Another option is to explore an Advanced Practice Provider’s residency or fellowship program. These are often one- to two-year programs that provide specialized training with patient populations, including, but not limited to, critical care, oncology, and cardiac surgery (SCCM, 2025).
No matter which you choose, you will also want to find out if your department or hospital has a formal mentorship program. This may be your preceptor for orientation, your supervisor, or an advanced practice program that is systemwide. If none of those exist, professional organizations also offer these types of opportunities. It helps to have a support system you can turn to ask questions, seek insight, feedback, and recommendations for success as you evolve as a new nurse practitioner and beyond.
Once I become a nurse practitioner, is that it?
The short answer to this question is … it’s up to you. It will take time to transition to practice, and I think most of my colleagues would agree with me in saying it will be at least a year before you understand what you are doing, and another year to be competent in what you are doing. Now that’s not to say you haven’t been prepared academically, and you will have an orientation process, but it takes time to learn the role and master the skill set — and that is OK.
My advice would be to take your time settling into the role and then consider your path of professional development. This may be moving along a leadership pathway; further education such as a Ph.D., DNP, or MBA; or transitioning to less clinical practice and into academia to teach. Attend conferences, expand your professional network, see how others have directed their careers. Then find your niche, what ignites your spark and your passion, and the possibilities are endless.
What is one piece of advice you would give to students who are exploring schools and interested in becoming a nurse practitioner?
Ask your college or university upfront about the clinical placement process, even if it is during the exploration or interview process. Find out if (a) you are required to find your own clinical preceptors through your professional network or other students, as “cold-calling” or “cold-emailing” is generally frowned upon, or (b) the college or university will assist you in this process.
In the event the latter is true, the next question should be how close or far from home a placement could be. In some cases, placements can be two or more hours one way from your residence, and you want to consider the time commitment, as this will be around an 8- to 12-hour shift, multiple days a week, outside of coursework and your personal life. Additionally, don’t hesitate to ask about the ability to form a collaborative agreement with a hospital or system closer to your home to make clinical experiences easier to facilitate for you and your support system.
It is important to know this information early because clinicals can be a very stressful time for you as a student, and the extra baggage of trying to find a preceptor and commuting time can hopefully be put to a minimum.
Conclusion
As you continue to explore the role of the nurse practitioner, the most essential piece of advice of all is ensuring that this career, the educational offerings, and all that comes after are what works best for you. Just like in nursing, we all have a different story to tell on how we got to where we are today, so don’t be afraid to ask others about their journey, seek their advice, shadow on the job, and find the role that best suits you!
References
- History of nursing
- Historical Timeline of the Nurse Practitioner
- Spitzer, W. O., Sackett, D. L., Sibley, J. C., Roberts, R. S., Gent, M., Kergin, D. J., Hackett, B. C., Olynich, A., Hay, W. I., Lefroy, G., Sweeny, G., Vandervlist, I., Nielsen, H. S., MacKrell, E. V., Prowse, N., Brame, A., Fedor, E., & Wright, K. (1974). The Burlington Randomized Trial of the Nurse Practitioner. New England Journal of Medicine, 290(5), 251-256. https://doi.org/10.1056/nejm197401312900506
- What's a Nurse Practitioner (NP)?
- Report of the APRN Joint Dialogue Group Based on the Work of the APRN Consensus Group and the NCSBN APRN Committee
- Updated resource: Davis, W., Stanley, J., Buck, M., Walters, E., & DeGarmo, S. (2024). LACE and the APRN Consensus Model: Implications for Advancing Nursing Practice. AACN Advanced Critical Care, 35(1), 20–28. https://doi.org/10.4037/aacnacc2024956
- https://www.aacnnursing.org/essentials/tool-kit/faqs
- McLaughlin, D., Ricker, M., Abide, A., Bakshi, V., Bane, T., Bhullar, S. K., Boling, B., Byrd, C., Farley, T., Fuller, T. E., Gunville, C., Hogan, B. J., Newman, C., Nugent, K. L., Pandya, K. A., Peacock, S., Pisa, M., & Meissen, H. H. (2026). Recommendations for Advanced Practice Provider Postgraduate Training Programs in the United States: A Work Product of the Advanced Practice Provider Postgraduate Training Task Force of the Society of Critical Care Medicine. Critical Care Medicine. https://doi.org/10.1097/CCM.0000000000007061
Content published on the Medical-Surgical Monitor represents the views, thoughts, and opinions of the authors and may not necessarily reflect the views, thoughts, and opinions of the Academy of Medical-Surgical Nurses.